Sleeping with Shoulder Pain
Disclosure: By clicking on the product links in this article, Mattress Nerd may receive a commission fee at no cost to you, the reader. Read full disclosure statement.
Mattress Nerd consulted Vivian Eisenstadt, MAPT, CPT, MASP, to ensure that this article met our editorial standards
Shoulder pain is surprisingly common and can range from being slightly bothersome to excruciating. The condition can limit mobility and sideline even the fittest of individuals, often interfering with sleep. Continue reading to learn how you can manage your shoulder pain for a better night’s rest!

Is Your Sleep Position to Blame for Your Shoulder Pain?
While the notion that shoulder pain (or pain of any kind for that matter) can interrupt our sleep is not rocket science, many fail to realize that the relationship between pain and sleep is a reciprocal one. So, while your shoulder pain may be the reason you just can’t seem to fall asleep when your head hits the pillow, the way you sleep may be the culprit for your shoulder pain, causing what can feel like an endless cycle of lackluster sleep and constant discomfort. We understand lack of sleep is a sacrifice one should not be willing to make and we are here to help. Let’s start by developing a better understanding of shoulder pain.
Understanding Shoulder Pain
The shoulders are complex structures made up of several joints combined with tendons and muscles that enable the shoulders to move with almost 360 degrees of motion. With more than a dozen muscles working together, our shoulders allow us to raise, twist, and move our arms. But when we injure a shoulder, the associated pain causes us to lose much of that range of motion.
Most shoulder problems are caused by inflamed or torn tendons, bursitis, rotator cuff injuries, osteoarthritis, or fractures. Rarely, the source of the pain can be tumors, infection, or nerve-related problems.
But if you prefer to sleep on your side — as most people do — then your sleeping position could be to blame. That’s because sleeping on your side places additional pressure on your shoulder that can cause irritation and pain and worsen injuries.
Ways to Alleviate Shoulder Pain for Better Sleep
Shoulder pain isn’t something you can just shrug off. Consider these strategies to prevent causing or worsening shoulder pain.
#1 Adjust Your Sleep Position
This may sound like a no-brainer, but you can avoid or at least decrease your shoulder pain by not sleeping on your sore shoulder. This lets your shoulder heal and helps prevent further damage.
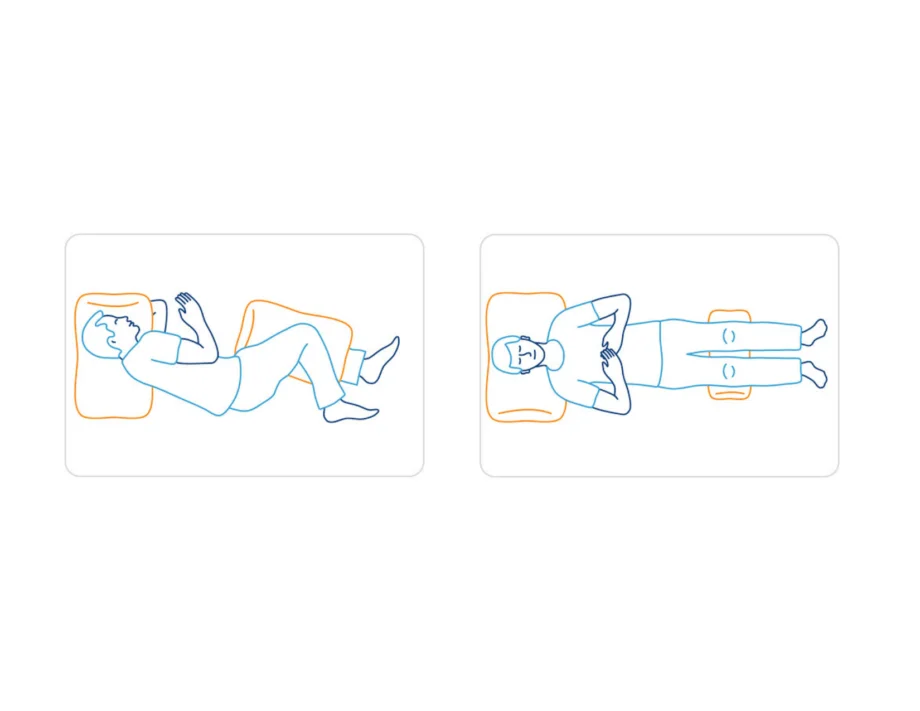
The orthopedic doctors at Ortho Bethesda recommend two sleeping positions for people dealing with shoulder pain—sleeping on the opposite side of your body or sleeping on your back.
If you prefer to sleep on your side, be aware that you may cause pain to your other shoulder if your mattress is too firm.
You’ll also want to be sure your head is propped up with a pillow that has a high enough loft to keep your spine aligned. Otherwise, you can strain your neck. If you can manage, try sleeping on your back to reduce pressure on your shoulders and keep your spine in a neutral position.
#2 Avoid Overuse
The American Academy of Orthopaedic Surgeons suggests using some common sense and stop doing those repetitive movements that put stress on your muscles and cause joint pain. That includes avoiding overexertion and overdoing activities you normally don’t participate in. It sounds easy enough, but putting it into practice takes some mindfulness, especially if your pain isn’t a constant reminder and only flares up when you overuse it.
#3 Keep It Moving
Just because your shoulder is sore doesn’t mean you should skip out on all exercise. A strong, healthy body is better equipped to resist injury, recover faster, and handle repetitive movements with ease. Remember, the four pillars of good health include exercise, a nutritious diet, mental health and good sleep.
#4 Stretch It Out
Yoga is a great way to relieve stress and help you sleep better in general. It also keeps joints limber, which helps prevent injury and restore function. Tight muscles also tear more easily and can cause shoulder pain. Stretching exercises especially before workouts help loosen muscles and reduce your risk of injury.
#5 Consider Pain Relievers
Medications can help take the edge off your pain and help you sleep. Over-the-counter medications, such as acetaminophens like Tylenol or nonsteroidal anti-inflammatory drugs (NSAIDs) like Advil or Motrin should be your first-line options. If your pain cannot be controlled with OTC medicines, contact your doctor about other options.
#6 Look Into Your Mattress
Your sleeping surface has a lot to do with your quality of sleep, especially if you suffer from shoulder pain. If your mattress doesn’t have enough cushioning and support, it can worsen or even cause shoulder pain.
According to a study published in the journal Applied Ergonomics, participants with back and shoulder pain experienced “progressive improvement” in pain while sleeping after switching out their old mattress for a newer one. The mattresses study participants used were made with memory foam or latex — two mattress materials that provide plenty of cushioning at the sensitive pressure points of the shoulders and hips with enough support to keep the spine aligned and prevent backaches.
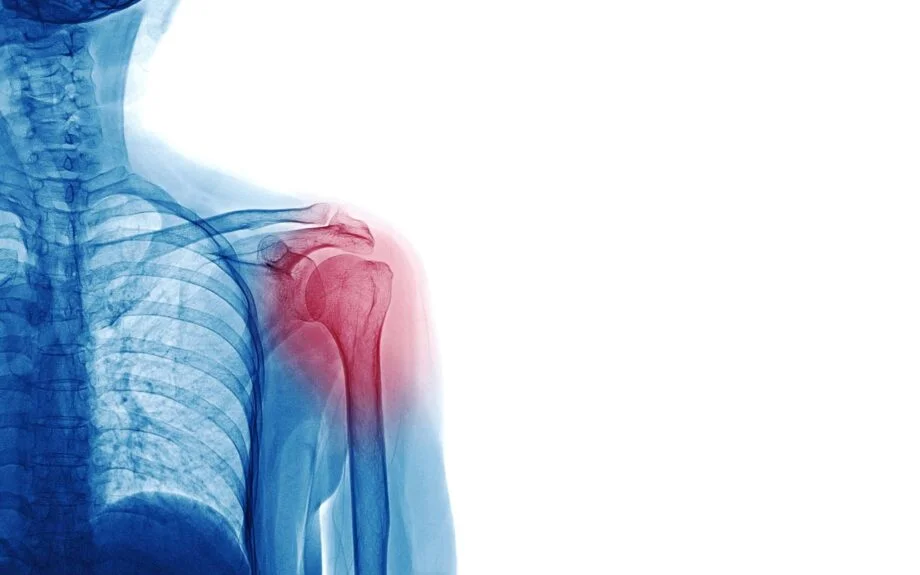
Additional Contributors to Shoulder Pain at Night
Sleeping on your side or with your arm over your head can irritate and inflame your shoulder joint and cause pain. But there are other conditions that cause shoulder pain.
Injuries and Medical Conditions
- Rotator cuff injuries affect the group of muscles and tendons that surround the shoulder joint and keep the head of your upper arm bone in the shoulder socket. The rotator cuff can become injured or torn from injuries (such as falls or accidents) or degeneration due to aging. Rotator cuff injuries feel like a dull ache deep in the shoulder that worsens during movement, such as when you change positions while sleeping.
- Repetitive use injuries: Repetitive, prolonged, or awkward movements of the shoulder can cause shoulder tendonitis. In fact, repetitive use injuries are among the most common injuries in the country, causing more than half of all athletic-related injuries. Shoulder tendonitis occurs when the tendons become inflamed. The classic symptoms include a toothache-like pain that radiates from the outer arm to several inches below the shoulder. Some people report waking from a sound sleep with a nagging pain in the upper arm.
- Bursitis of the shoulder: Bursitis is the inflammation of a bursa sac, the small fluid-filled pouches or sacs found over areas where friction occurs. Bursitis of the shoulder happens at the top of the arm bone and tip of the shoulder, where the tendons of the rotator cuff and the bursa lie. When shoulder bursa become inflamed, they can cause swelling and redness on the shoulder and mild, constant pain.
- Shoulder impingement syndrome is similar to bursitis of the shoulder. It occurs when the top of the shoulder blade presses or rubs against the tendons and bursa. It causes sudden shoulder pain when you lift your arm overhead or backward, and can awaken you at night if you tend to toss and turn when you sleep.
- Osteoarthritis of the shoulder: Osteoarthritis (OA) is the most common type of arthritis. This degenerative joint disease occurs when flexible cartilage in the joint wears down. OA occurs most often in the hands, hips, and knees, but can also affect the shoulder. The Arthritis Foundation estimates that nearly 1 in 3 people over the age of 60 suffers from shoulder OA to some degree. Shoulder osteoarthritis feels like a deep ache in the joint that is aggravated by activity and becomes progressively worse.
- Frozen shoulder is characterized by pain and stiffness at the shoulder joint. It most often occurs in people with diabetes as well as those who have kept their arm immobilized for a long period of time due to surgery. Frozen shoulder begins with a “freezing stage” during which any movement of the shoulder causes pain and limits motion. During the “frozen stage” pain begins to lessen but the shoulder becomes stiffer and more difficult to use. After a year or two, is the “thawing stage,” when the range of motion begins to improve. For some, the pain of frozen shoulder worsens at night.
When to Get Help
Seek medical attention if you experience any of the following symptoms with shoulder pain:
- Sudden onset of acute pain in the shoulder.
- Pain that persists for days especially after trying at-home fixes.
- Weakness in the shoulder or inability to lift the arm.
- Abnormal feeling in the arm, hand, or fingers.
- A significant loss in range of motion.
- If shoulder pain follows an accident or fall.
- If nighttime shoulder pain disrupts sleep.
- If there are signs of infection such as swelling, redness, inflammation, or extreme pain at the shoulder, or if shoulder pain is accompanied by a fever or fatigue.
Final Thoughts
Shoulder pain shouldn’t be shrugged off, especially if it interferes with your sleep. While you will want to get a proper diagnosis from a medical professional, there are some strategies you can put into action to reduce or prevent shoulder pain, such as limiting repetitive use, exercising and stretching, and paying closer attention to your sleeping position. You may also want to invest in a new mattress. A mattress that is too firm or doesn’t have enough support can cause or worsen shoulder pain, especially if you’re a side sleeper.
Meet Our Medical Reviewer
Vivian Eisenstadt, MAPT, CPT, MASP Vivian Eisenstadt is the founder of Vivie Therapy. Her private practice helps individuals with chronic and recent pain reclaim their lives quickly and thoroughly. Prior to founding her own practice, Vivian served as a Physical Therapist at Cedars-Sinai Medical Center. She specialized in treating spinal injuries, postural dysfunctions, sprains and strains, and general orthopedic injuries.


