Sleep & Juvenile Arthritis
Disclosure: By clicking on the product links in this article, Mattress Nerd may receive a commission fee at no cost to you, the reader. Read full disclosure statement.
Juvenile arthritis (JA), also called pediatric rheumatoid disease, refers to inflammatory and rheumatic diseases that develop in children before the age of 16. Most are autoimmune or autoinflammatory diseases that typically cause joint inflammation, swelling, pain, and tenderness. Some types of JA have few or no joint symptoms and only affect the skin and internal organs.
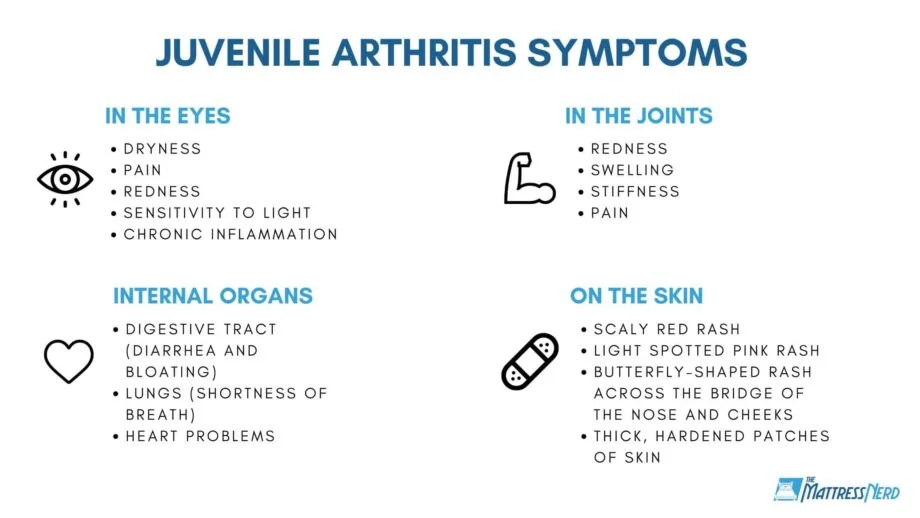
Different Types of Juvenile Arthritis
There are four common types of juvenile arthritis:
Juvenile idiopathic arthritis: This is the most common form of juvenile arthritis. It typically causes joint pain and inflammation. There are six types of juvenile idiopathic arthritis:
- Oligoarthritis: The most common, this affects four or fewer joints, typically larger ones such as the knees or elbows.
- Polyarthritis: Affects five or more joints, often on both sides of the body.
- Systemic: Affects the entire body including joints, skin, and internal organs. Symptoms may also include rash or fever that lasts at least two weeks.
- Psoriatic arthritis: Includes joint symptoms and a scaly rash behind the ears and/or eyelids, elbows, knees, belly button, and scalp.
- Enthesitis-related: Also called spondyloarthritis, this condition affects where the muscles, ligaments, or tendons attach to the bone, such as at the hips, knees, and feet. In some cases, it may also affect the digestive tract (diagnosed as Crohn’s disease or ulcerative colitis) and lower back (diagnosed as ankylosing spondylitis).
- Undifferentiated: These symptoms don’t align with any other JA subtype but inflammation is present in at least one or more of the joints.
Juvenile lupus: An autoimmune disease that can affect the joints, skin, and internal organs, including the heart, lungs, nervous system, and kidneys.
Vasculitis: This condition causes inflammation of the blood vessels, which can lead to heart complications. The most common types of vasculitis seen in kids and teens are Kawasaki disease and Henoch-Schonlein purpura (HCP).
Juvenile myositis: An inflammatory disease that causes muscle weakness.
Juvenile scleroderma: Describes a group of conditions that causes the skin to tighten and harden.
Fibromyalgia: A chronic pain syndrome that can cause widespread muscle pain and stiffness, fatigue, disrupted sleep, and other symptoms.
Juvenile arthritis is often controlled with medications. In most cases, the disease can go into remission for months, years, or even the rest of the person’s life, often with little or no permanent joint damage. However, some children with JA grow up to become adults with arthritis.
How Juvenile Arthritis Can Interfere with Sleep Quality
Sleep is essential to our physical, mental, and emotional health, and it is especially vital for children and teenagers whose bodies and brains are still developing. A good night’s sleep better equips them to pay attention in school, retain information, and be active. But kids who suffer from juvenile arthritis have certain challenges that can interfere with sleep. According to Dr. Chris Norris of SleepStandards, “There is a strong relationship between pain and sleep quality. Children who experience more pain, on average, also report poor sleep. Interestingly, other factors, including the number of joints affected and overall disease severity, do not correlate with sleep quality.”
Chronic Pain
It can be difficult to get children to settle down for bedtime when they are healthy. But it can be especially challenging if they suffer from pain. Equally frustrating is that inadequate sleep can actually worsen a person’s perception of pain. A study published in the journal BMC: Pediatric Rheumatology found that kids who sleep poorly experience increased symptoms related to juvenile arthritis. As a result, their sleep quality may suffer.
Depression / Sleep-Related Anxiety
Chronic pain has been linked to depression and anxiety, both of which can hinder sleep. A study by psychology researchers at the University of North Carolina at Chapel Hill found that children with juvenile idiopathic arthritis were more likely to suffer from depression. Those children also reported sleeping poorly at night. It’s difficult to discern whether pain and poor sleep are the cause of depressed mood, or whether depressed mood worsens pain and sleep. Researchers theorize it is a combination of both.
Sleep Disordered Breathing
Obstructive sleep apnea, or OSA, is a potentially serious condition that affects an estimated 22 million American adults. But it can also affect kids. OSA occurs when breathing stops intermittently for several seconds during the night because the soft tissues in the mouth have blocked the airway. In severe cases, OSA can cause a drop in blood-oxygen levels and interrupt sleep, leading to learning, behavior, growth, and heart problems.
According to researchers with the University of Washington, as many as 40% to 50% of school-age children with juvenile idiopathic arthritis have obstructive sleep apnea compared to healthy children of the same age. In most cases, parents and caregivers are unaware their child has OSA. The study also found that children with JA and OSA were more fatigued and had less quality of life compared to children with JA without sleep apnea.
There is no definitive answer as to why children with juvenile arthritis are more prone to sleep apnea. One theory is that they have a higher prevalence of arthritis in the temporomandibular joint, or TMJ (near the jaw), which may impair the growth of the mandibular and thus restrict breathing during sleep resulting in OSA.
Tips For Getting Better Sleep with Juvenile Arthritis
Skip the nap: For children age 4 or older, consider skipping the afternoon nap. Daytime napping can interfere with bedtime. If a rest is necessary, try to limit it to 20 minutes.
Exercise: Being active during the day with some type of cardiovascular exercise can improve sleep. However, if your child’s disease limits their mobility, talk to their doctor about appropriate activities. According to Dr. Aragona, “Slower exercise will do better than fast, intense ones. Walking or slow jogging may be better than running. Stretching these areas will also help strengthen them.”
Cut out caffeine in the afternoon and evenings: Caffeine even late in the day can make falling asleep at night difficult for some children.
Adopt a bedtime routine: Children of all ages — and even adults — can benefit from a bedtime routine. Start about 30 minutes before bedtime and choose calming activities like warm baths, bedtime stories, or soothing music.
Upgrade your child’s mattress: Children with chronic pain can sleep better in a memory foam mattress that is supportive yet comfortably contouring. Foam mattresses also provide relief at pressure points such as the hips and shoulders. “When the child is going to sleep, make sure that there is little inflammation in the joints, and they lay as still and as flat as they can. This should help with the position while sleeping. As for pain, if it is unbearable and they cannot sleep, maybe steroid cream or anti-inflammatory medication could help also,” says Dr. Aragona, General Practitioner & Family Doctor at Prescription Doctor.
Establish a daytime routine: Some children thrive better with regular bedtimes and wake times, even on weekends.
Limit electronics: Video games and other electronic devices before bedtime can hinder sleep. Be sure your child’s bedroom is free of these attractive nuisances.
Schedule medications: Some medications can interfere with your child’s ability to fall asleep. If your child is on medications that disturb sleep, like prednisone or hydroxychloroquine, administer them earlier in the day, if possible.
Avoid big meals before bedtime: Full bellies are not conducive to sleep. Try to serve dinner well before bedtime so little bellies have plenty of time to digest.
Cognitive-behavioral therapy: Talk therapy can help children and teenagers work through anxiety, depression, and general frustrations with their limitations, and can help reduce symptoms of insomnia.
Sleep Tips For Juvenile Arthritis Caregivers
Sleep isn’t just a problem for children with juvenile arthritis. Their parents and caregivers can lose sleep as well and should take extra precautions to ensure they get plenty of rest. But parents and caregivers of children with JA have their own challenges related to their child’s disease including reduced sleep time, increased arousals from REM sleep, insomnia, and sleep deprivation. These conditions can lead to immune and cardiovascular effects, as well as psychological distress. Parents and caregivers are also susceptible to burnout syndrome, depression, and diminished quality of life, which can adversely impact their caregiving.
Create an environment for sleeping, not caregiving. This room should be your sanctuary reserved for relaxing and sleeping, not taking care of others. Choose bed linens that are soft and regulate your temperature, and consider upgrading your mattress. A memory foam, latex, or hybrid mattress can help cradle your sore body and relieve aches and pains so you wake feeling refreshed and able to carry out your caregiving duties.
Schedule time to worry. It doesn’t help to worry constantly. But you cannot dismiss your concerns. Set a timer and literally take time to worry. Use the time to write down your concerns in a journal. When the timer signals your “anxious hour” is over, put your notes away and get on with your day.
Establish a bedtime routine. A nighttime routine helps children settle down for bedtime, but it can also help you relax and prepare yourself to sleep. Try taking a warm bath or listening to soothing music, relaxing under a weighted blanket, or meditating about 30 minutes before bedtime. And put away electronic gadgets that stimulate your mind instead of prepare you for sleep.
Meditate. Relaxation exercises, self-hypnosis, and meditation can help you clear your mind of anxiety and worry so you can fall asleep and stay asleep.
Therapy. Cognitive-behavioral therapy is great for helping children and teens come to terms with their disability and help them sleep. It can also help caregivers deal with their own angst, which can help you sleep better.


